COLORECTAL (BOWEL) CANCER
Colorectal cancer is experienced by around 5% of the Australian Population. Colorectal cancer is the unregulated growth in the colon or in the rectum usually starting from a polyp in the bowel.
Bowel cancer, also known as colorectal cancer, can affect any part of the colon or rectum; it may also be referred to as colon cancer or rectal cancer, depending on where the cancer is located.
The colon and rectum are parts of the large intestine. The colon is the longest part of the large intestine (the first 1.8 metres). It receives almost completely digested food from the ceacum (a pouch within the abdominal cavity that is considered to be the beginning of the large intestine), absorbs water and nutrients, and passes waste (stool/faeces/poo) to the rectum.
Causes
There are two kinds of risk factors or causes for bowel cancer – those that can be changed (modifiable) and those that cannot (non-modifiable). Modifiable; Bowel Cancer risk is increased by smoking, being overweight or obese, drinking alcohol, eating processed meats (smoked, cured, salted or preserved) or charred red meat.
These risks can be minimised through diet and lifestyle changes and are referred to as modifiable. Non Modifiable: Age, family history, hereditary conditions and personal health history can also influence bowel cancer risk. These factors cannot be changed. People with certain diseases and illnesses seem to be more prone to developing bowel cancer. These include Type II diabetes, other forms of closely linked cancer such as ovarian or digestive system cancers, and inflammatory bowel diseases (IBD) including Crohn’s and Ulcerative Colitis.
A person’s risk category also depends on how many close relatives have bowel cancer and their age at diagnosis. Someone with several close relatives diagnosed with bowel cancer before age 50 has a much higher risk than someone with no close relatives with bowel cancer. In some family members, bowel cancer develops due to an inherited gene mutation.
Symptoms
During the early stages of bowel cancer, people may have no symptoms, which is why screening is so important. Screening can be done at home is easy and safe. National bowel screening program is a government initiative for people aged between 50-74.
The risk for the individual increases dramatically for the age of 50. If you are outside the ages please consult with your GP if you have concerns.
If you have any of the following symptoms for more than two weeks then it is advisable to see your GP. Blood from your bottom or in
your stools. ( blood in your poo) A change in your bowel habit whether this be persistent or intermittent for no reason (constipation,
diarrhoea or feeling you are not completely emptying your bowels) A change in the appearance of your stools, a change in the shape of
your poo; smaller, narrower or has mucous.
Pain in your abdomen or swelling. Pain in your rectum or anus. Non intentional weight loss, weakness or anaemia.
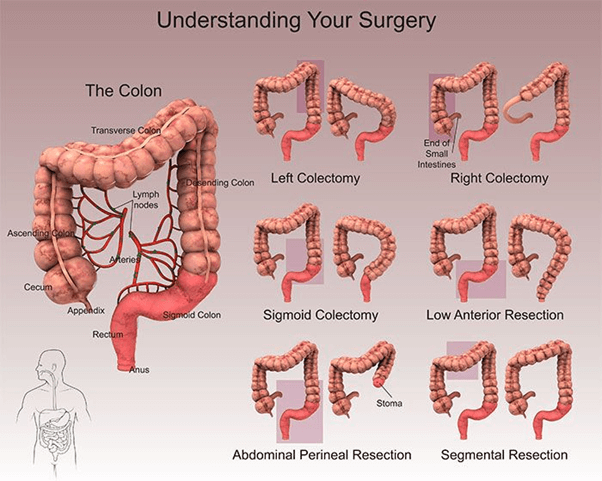
Colectomy
What is a Colectomy
Colectomy is surgery to remove part of the colon that is diseased. This can be performed ‘laparoscopically’ (keyhole surgery)or as an ‘open procedure’ The need for a Colectomy may be from cancer of the colon, inflammatory bowel disease such as Chron’s and ulcerative colitis, blocked bowel, a hole or tear in the bowel wall, repeated diverticulitis, fistula, precancerous polyps.
Types of Colectomy